Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.
sizing guide
Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.
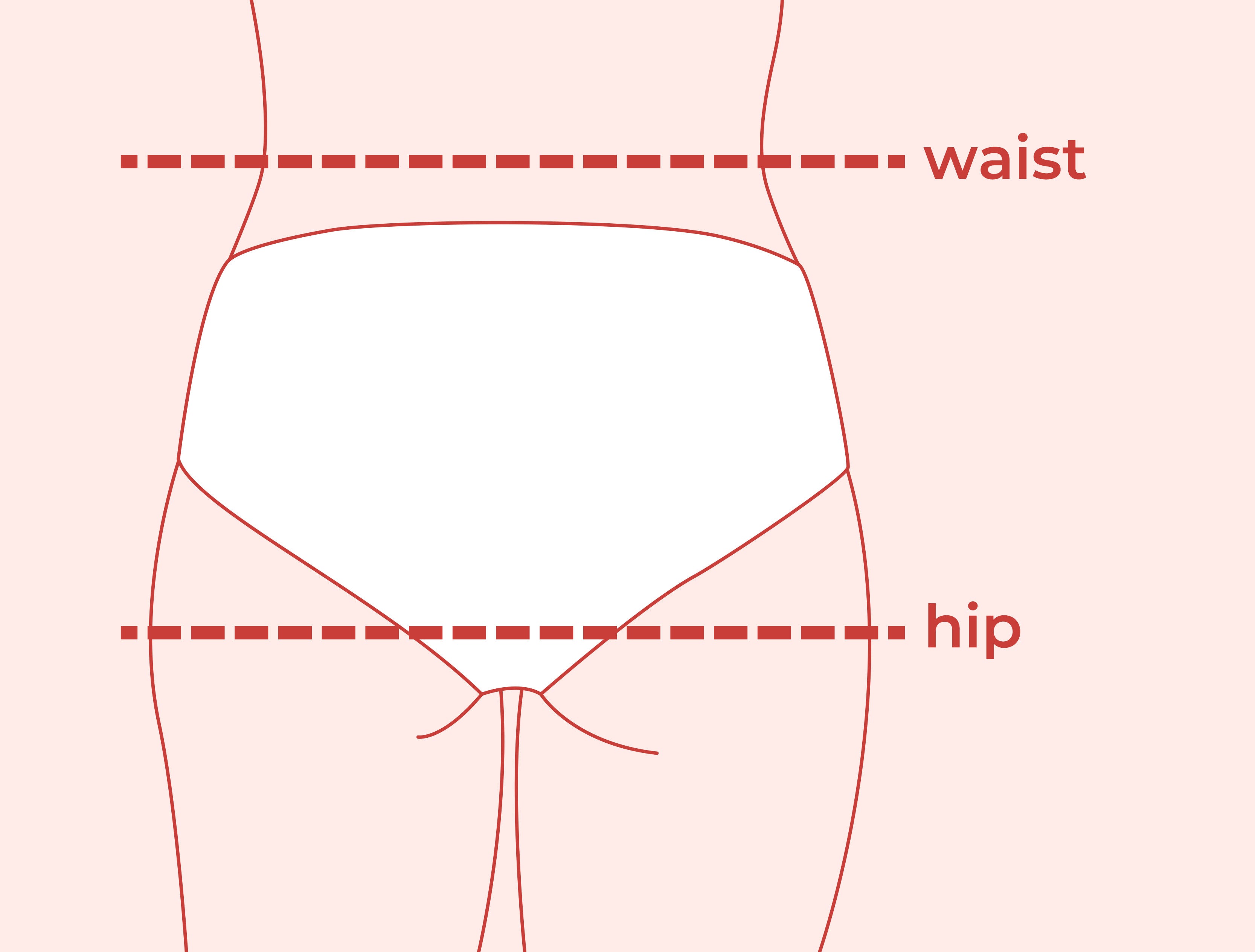
Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.

Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.

Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.

Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.

Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.

Measure around your body as shown.
If your measurements fall into different size categories, your hip measurement will be most accurate.

